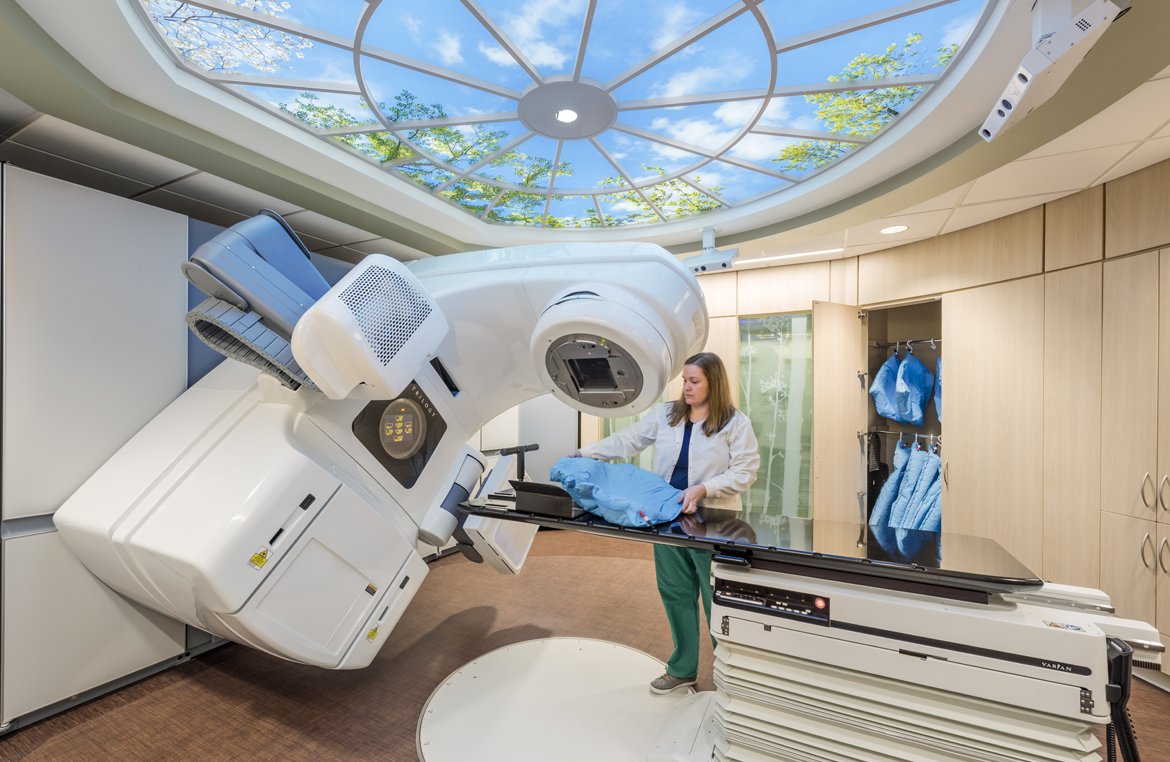
Linear accelerators are medical devices that are used for radiation therapy to treat cancer and other diseases. They work by generating high-energy X-rays or electrons that are targeted precisely at the tumor to control or destroy the cancer cells. With advancements in technology, modern linear accelerators have become an important tool in the fight against cancer and are able to deliver radiotherapy treatments effectively with minimal side effects.
How does a linear accelerator work?
A linear accelerator consists of a linear particle accelerator mounted on a gantry within an vault. Microwave generators located at either end of the accelerator tube power the device and produce electric fields that accelerate electrons to high speeds. As electrons travel down the length of the tube towards the tumor target area, they gain tremendous kinetic energy from these oscillating electric fields.
When the high-energy electrons hit their target, which is a piece of high-atomic number metal like tungsten, they slow down very rapidly. Most of the kinetic energy is converted into high-energy electromagnetic radiation in the form of X-rays. The generated X-rays emerge as a narrow beam from the target and penetrate the patient’s skin and tissue to precisely irradiate the tumor volume.
Linear accelerators are capable of producing X-ray energies ranging from 4 MeV to 25 MeV. The higher the energy of the X-rays, the deeper they can penetrate into the body. This penetration depth can be adjusted by altering the energy of the electron beam. The rapid deceleration of electrons and generation of X-rays occurs in a tiny fraction of a second, producing up to thousands of X-ray pulses per minute.
Advantages of linear accelerators
Linear accelerators have several advantages over traditional radiation sources like radioactive materials:
– Precision targeting: With image guidance technologies integrated into treatment planning and delivery systems, linear accelerators allow oncologists to precisely target irregularly shaped tumors with tight margins and minimize damage to surrounding healthy tissues. This enhances treatment effectiveness.
– Minimally invasive: Being non-invasive, linear accelerator treatments do not require surgery or implanted radioactive sources. Patients can continue their daily activities during and after a course of external beam radiotherapy.
– Dose flexibility: The dose rate can be varied during a treatment session based on the tumor type and nearby organs at risk. This allows protection of critical structures while still achieving tumor control.
– No radiation remains: Unlike radioactive sources which leave residual activity in the patient’s body, linear accelerators produce radiation only during treatment time, with no remaining radiation post procedure.
– Adaptive radiation treatments: Modern linear accelerators are equipped with onboard imaging like cone beam CT. This enables verification of patient position and size changes during a treatment course. The plan can then be adapted to ensure accurate dose delivery to the updated target.
Linear accelerator applications
Based on their versatility and precision, linear accelerators have become the primary choice for delivering certain radiation therapy treatments:
– Whole and half brain radiotherapy: Used extensively for brain tumors due to the ability to target irregular shapes near critical structures like optical nerves and cochlea.
– Head and neck cancers: Due to complex tumor shapes near vital organs like optic chiasm and brainstem, intensity modulated radiation therapy with linear accelerators enables safe dose escalation.
– Breast cancer: Widely used in post-surgical cases for regional nodal treatment and accelerated partial breast irradiation. Precise targeting reduces heart and lung doses.
– Lung cancer: Stereotactic body radiotherapy with linear accelerators delivers very high ablative doses to early stage lung tumors in a few fractions, minimizing lung tissue damage.
– Prostate cancer: Intensity modulated plans ensure coverage of the prostate gland and seminal vesicles while avoiding rectal toxicity. This has made radiotherapy a popular primary or adjuvant treatment option.
Advanced treatment techniques
Newer linear accelerator technologies continue to expand treatment capabilities and improve clinical outcomes:
– Volumetric modulated arc therapy (VMAT): Dynamic movement of the gantry and dose rate during treatment enables ultra-fast highly modulated arcs around the patient for complex plans in a few minutes.
– Stereotactic radiosurgery (SRS): Using multiple static convergent beams or dynamic arcs, SRS can precisely deliver ablative doses (500-2000 cGy) in 1-5 fractions to small intracranial lesions or certain extracranial tumors.
– Proton beam therapy: Select linear accelerators can accelerate protons to very high energies for particle beam radiotherapy. Protons deposit most dose at a finite depth, sparing deeper tissues completely.
– MR-linear accelerator systems: Combined with a magnetic resonance imaging device inline, these allow treatment adaptation based on daily onboard MRI scans for true image-guided treatments.
– FLASH radiotherapy: Some research explores using ultra-high dose rates from linear accelerators to exploit a proposed biological mechanism for safer high-dose treatments.